Introduction
Tuberculosis (TB), a highly contagious bacterial infection caused by Mycobacterium tuberculosis, remains a significant global health concern, affecting millions worldwide. Despite medical advancements, TB continues to challenge healthcare systems, necessitating comprehensive understanding and effective management strategies. This article delves into the multifaceted aspects of TB, from its epidemiology and transmission to diagnosis, treatment, and prevention measures.

Understanding Tuberculosis, Epidemiology and Global Impact, The Magnitude of the Problem
Tuberculosis persists as one of the top infectious killers globally, with an estimated 10 million new cases reported annually.
High-Burden Regions
Regions with limited access to healthcare, poverty, and overcrowding often experience a higher prevalence of TB, emphasizing the socio-economic determinants of the disease.
Impact on Vulnerable Populations
Vulnerable populations, including those living with HIV/AIDS, malnourished individuals, and marginalized communities, bear a disproportionate burden of TB, exacerbating existing health disparities.
Transmission and Pathogenesis, Modes of Transmission
TB primarily spreads through the inhalation of respiratory droplets expelled by individuals with active pulmonary TB, highlighting the importance of infection control measures in healthcare settings and communities.
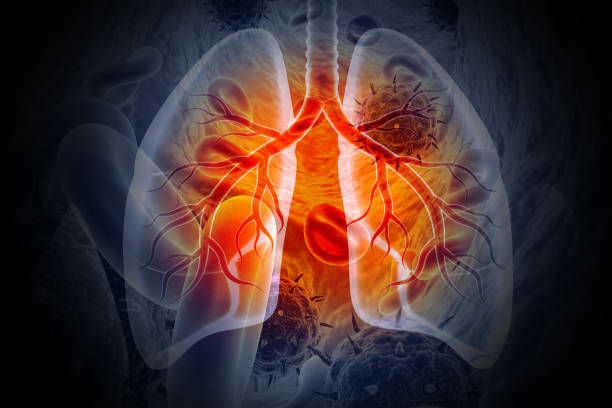
Pathogenesis
Upon inhalation, M. tuberculosis enters the lungs, where it evades the immune system by residing within macrophages, leading to the formation of granulomas and eventual dissemination to other organs.
Diagnosis and Screening, Clinical Presentation, Symptoms
Common symptoms of TB include persistent cough, fever, night sweats, weight loss, and hemoptysis, although asymptomatic cases and extrapulmonary manifestations pose diagnostic challenges.
Diagnostic Methods, Microbiological Tests
Sputum smear microscopy, culture, and molecular assays such as GeneXpert play pivotal roles in confirming TB diagnosis and detecting drug resistance.
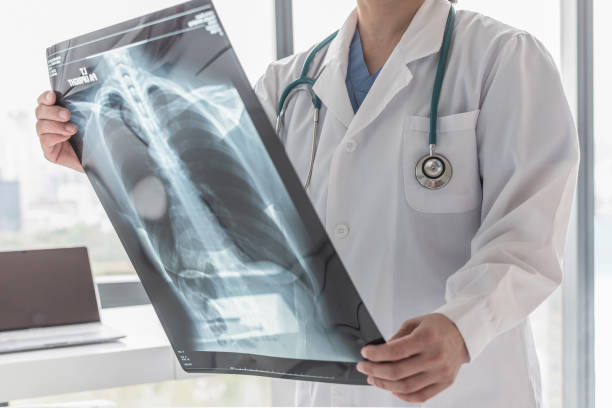
Radiological Imaging
Chest X-rays and computed tomography (CT) scans aid in assessing pulmonary involvement and identifying complications like pleural effusion and cavitation.
Screening Strategies, Contact Tracing
Identifying and screening close contacts of TB patients enables early detection of latent TB infection (LTBI) and active disease, curbing further transmission.
Mass Screening Campaigns
Community-based initiatives, including mobile X-ray units and TB awareness programs, contribute to identifying undiagnosed cases and promoting treatment adherence.
Treatment and Management, Antimicrobial Therapy, First-Line Drugs
The cornerstone of TB treatment involves a combination of antibiotics, including isoniazid, rifampicin, pyrazinamide, and ethambutol, administered over a specified duration to achieve cure and prevent drug resistance.
Drug-Resistant TB
Multidrug-resistant TB (MDR-TB) and extensively drug-resistant TB (XDR-TB) pose formidable challenges, necessitating prolonged treatment with second-line drugs and close monitoring to optimize outcomes.
Patient Support and Adherence, Directly Observed Therapy (DOT)
DOT programs ensure medication adherence by supervising treatment administration, addressing barriers to care, and providing psychosocial support to patients.
Nutritional Support
Optimal nutrition plays a crucial role in TB management, enhancing immune function and treatment response, particularly in malnourished individuals.
Prevention Strategies, Vaccination, Bacillus Calmette-Guérin (BCG) Vaccine
The BCG vaccine, although imperfect, remains a vital preventive measure, offering partial protection against severe forms of TB in children and reducing morbidity and mortality rates.
Infection Control Measures
Respiratory Hygiene
Promoting cough etiquette, adequate ventilation, and use of personal protective equipment minimizes TB transmission in healthcare and congregate settings.
Guidelines
TB primarily spreads through the inhalation of respiratory droplets expelled by individuals with active pulmonary TB. Common symptoms include persistent cough, fever, night sweats, weight loss, and hemoptysis. TB diagnosis relies on microbiological tests such as sputum smear microscopy and culture, along with radiological imaging and clinical evaluation.
The standard treatment regimen involves a combination of antibiotics, including isoniazid, rifampicin, pyrazinamide, and ethambutol, administered for a specified duration. While TB is preventable, comprehensive strategies encompassing vaccination, infection control measures, and early diagnosis and treatment are crucial in curbing its spread. TB is curable with appropriate antimicrobial therapy administered under direct observation and adherence to treatment protocols.
Conclusion
Tuberculosis remains a formidable global health challenge, demanding concerted efforts to mitigate its impact. By enhancing public awareness, implementing robust screening and treatment programs, and addressing socio-economic determinants, we can strive towards a TB-free world.