Introduction
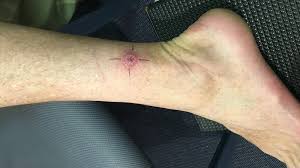
Buruli ulcer, a neglected tropical disease caused by the bacterium Mycobacterium ulcerans, poses a significant public health challenge in various regions worldwide. This comprehensive guide dives deep into ten effective solutions for combating Buruli ulcer, providing valuable insights and actionable strategies to address this debilitating skin condition.
Understanding Buruli Ulcer
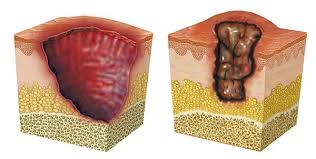
Buruli ulcer, also known as Bairnsdale ulcer or Daintree ulcer, primarily affects the skin and sometimes the bone, leading to severe tissue destruction if left untreated. This section delves into the etiology, transmission, and clinical manifestations of Buruli ulcer, shedding light on its impact on affected individuals and communities.
Etiology of Buruli Ulcer
The causative agent of Buruli ulcer, Mycobacterium ulcerans, belongs to the same family as the bacteria responsible for tuberculosis and leprosy. Understanding its mode of transmission and reservoirs is crucial for effective disease management.
Transmission Dynamics
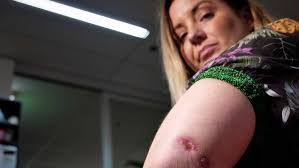
Buruli ulcer transmission often occurs through environmental sources, with stagnant water bodies serving as potential breeding grounds for the bacteria. Explore the intricate dynamics of disease transmission and the role of environmental factors in its spread.
Diagnostic Modalities for Buruli Ulcer
Accurate and timely diagnosis is paramount for initiating prompt treatment and preventing disease progression. This section discusses various diagnostic approaches and their significance in identifying Buruli ulcer cases.
Clinical Presentation
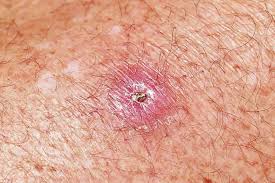
Recognizing the characteristic clinical features of Buruli ulcer, such as painless nodules, plaques, or ulcers with undermined edges, aids in early diagnosis and management. Dive into the nuances of clinical assessment and differential diagnosis.
Laboratory Investigations
From microscopy to PCR-based assays, laboratory techniques play a vital role in confirming Buruli ulcer cases and monitoring treatment response. Learn about the strengths and limitations of different laboratory tests in diagnosing this infectious disease.

Medical Management of Buruli Ulcer
Effective treatment strategies are essential for alleviating symptoms, preventing complications, and promoting recovery in individuals with Buruli ulcer. This section explores pharmacological and surgical interventions tailored to the needs of patients.
Antibiotic Therapy
Antimicrobial agents, such as rifampicin and clarithromycin, form the cornerstone of medical management for Buruli ulcer. Delve into the pharmacological mechanisms and treatment regimens recommended by healthcare providers.
Surgical Interventions
In cases of extensive tissue damage or complications, surgical procedures like debridement and skin grafting may be necessary to achieve optimal outcomes. Explore the role of surgical interventions in managing advanced Buruli ulcer lesions.
Wound Care and Rehabilitation
Comprehensive wound care and rehabilitation are integral components of Buruli ulcer management, aiming to promote healing, prevent disability, and enhance the quality of life for affected individuals. This section outlines evidence-based strategies for wound management and functional restoration.
Wound Debridement
Debridement of necrotic tissue and wound cleansing are essential for facilitating granulation tissue formation and reducing the risk of secondary infections. Discover the principles of effective wound debridement and the importance of regular monitoring.
Physiotherapy and Rehabilitation
Physiotherapeutic interventions, including range of motion exercises and strengthening techniques, play a crucial role in restoring function and mobility in individuals recovering from Buruli ulcer-related disabilities. Learn about the multidisciplinary approach to rehabilitation in this context.
Prevention and Control Measures
Preventive strategies and community-based interventions are vital for reducing the burden of Buruli ulcer and interrupting disease transmission cycles. This section highlights key initiatives aimed at prevention, early detection, and case management.
Health Education and Awareness
Raising public awareness about Buruli ulcer, its risk factors, and preventive measures is essential for promoting early recognition and seeking timely medical care. Explore innovative health education campaigns and community engagement strategies.
Environmental Sanitation
Improving water quality, sanitation infrastructure, and hygiene practices in endemic areas can contribute significantly to reducing the incidence of Buruli ulcer. Delve into the importance of environmental sanitation as a holistic approach to disease prevention.
Research and Innovation
Ongoing research efforts and innovation in Buruli ulcer diagnostics, treatment modalities, and disease surveillance are crucial for advancing our understanding and combatting this neglected tropical disease. This section explores recent developments and future directions in Buruli ulcer research.
Novel Therapeutic Approaches
From immunotherapies to topical antimicrobial agents, novel treatment modalities offer promising avenues for improving clinical outcomes and reducing treatment duration in Buruli ulcer patients. Stay updated on the latest advancements in therapeutic innovation.
Epidemiological Studies
Epidemiological studies provide valuable insights into the spatial distribution, risk factors, and transmission dynamics of Buruli ulcer, informing targeted intervention strategies and resource allocation. Explore the role of epidemiological research in disease surveillance and control.
Research Revelations Buruli:
Buruli ulcer is primarily transmitted through environmental sources, including stagnant water bodies contaminated with Mycobacterium ulcerans. Clinical manifestations of Buruli ulcer typically include painless nodules, plaques, or ulcers with undermined edges, often affecting the skin and sometimes the bone. Laboratory investigations such as microscopy, PCR assays, and culture techniques are employed for diagnosing Buruli ulcer and monitoring treatment response. The medical management of Buruli ulcer involves antibiotic therapy with agents like rifampicin and clarithromycin, along with surgical interventions in advanced cases. Preventive measures for Buruli ulcer encompass health education, environmental sanitation, early case detection, and community-based interventions aimed at interrupting disease transmission. Ongoing research and innovation in Buruli ulcer diagnostics, treatment modalities, and epidemiological studies are essential for advancing our understanding and addressing the challenges posed by this neglected tropical disease.
Conclusion
In conclusion, Buruli ulcer remains a significant public health concern, particularly in endemic regions where access to healthcare resources may be limited. By implementing evidence-based interventions, fostering research collaborations, and raising awareness, we can strive towards achieving the ultimate goal of eliminating Buruli ulcer as a global health threat.